One platform to manage credentialing cases, track expirations, submit claims, and watch your insurance revenue grow — in real time, 24/7.
See where every credentialing case stands, what's expiring, and how your claims are performing — the second you log in.
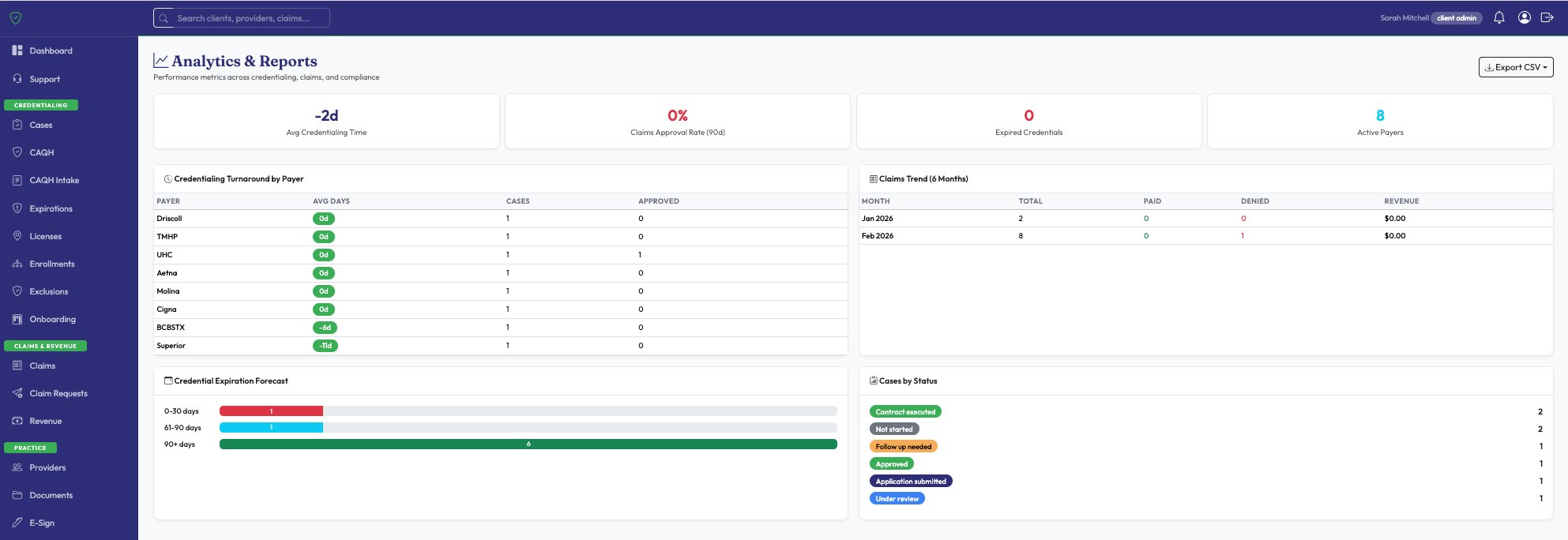
Each provider × payer combination tracked as a separate case with color-coded statuses. You always know exactly what's moving and what needs a push — across all 8 Texas payers.
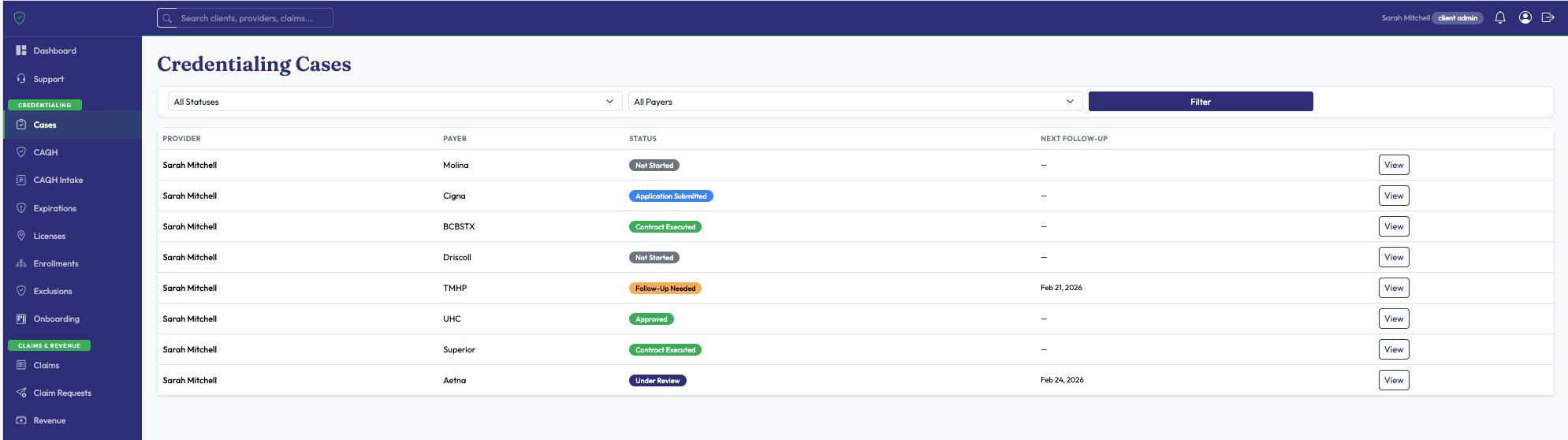
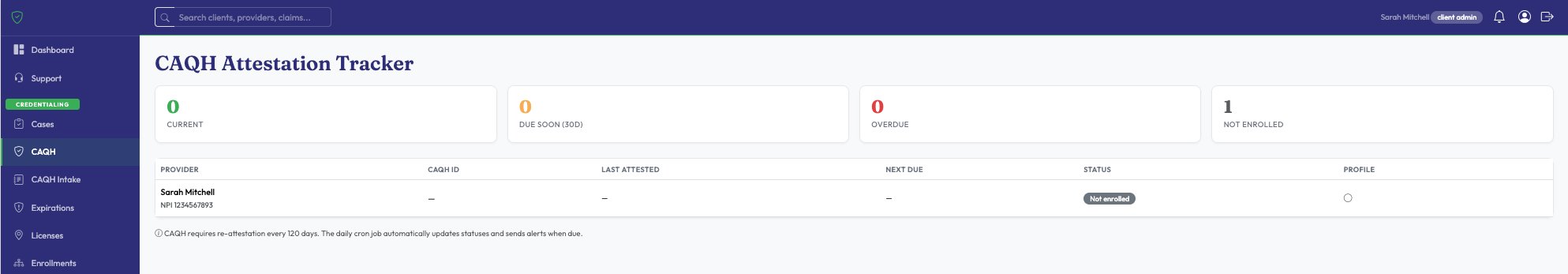
Licenses, insurance policies, CAQH attestations, payer re-credentialing — all tracked and color-coded. Automated email alerts fire at 90, 60, 30, 14, and 7 days before expiration.
One missed deadline can cost you months of revenue.
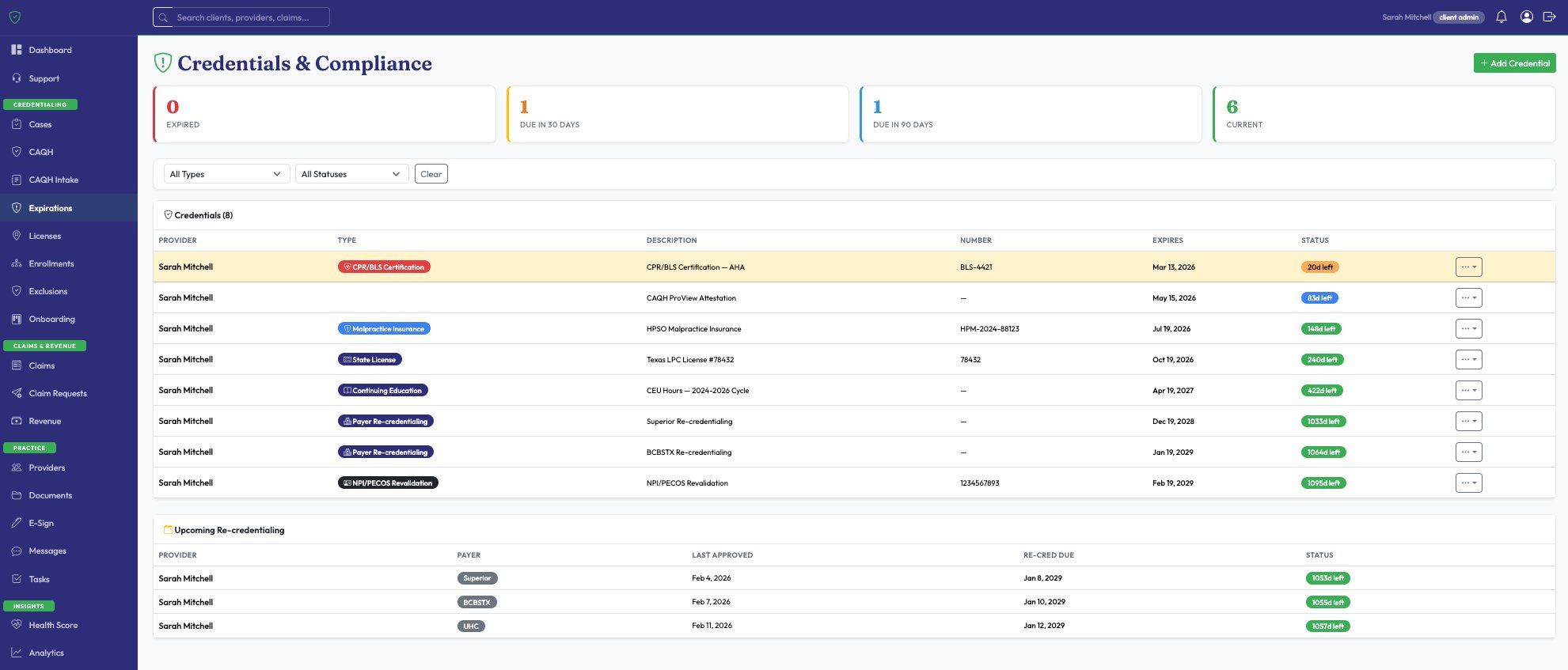
A single number tells you how healthy your compliance is. Scored across 5 dimensions with specific action items to improve. No other credentialing company offers this.
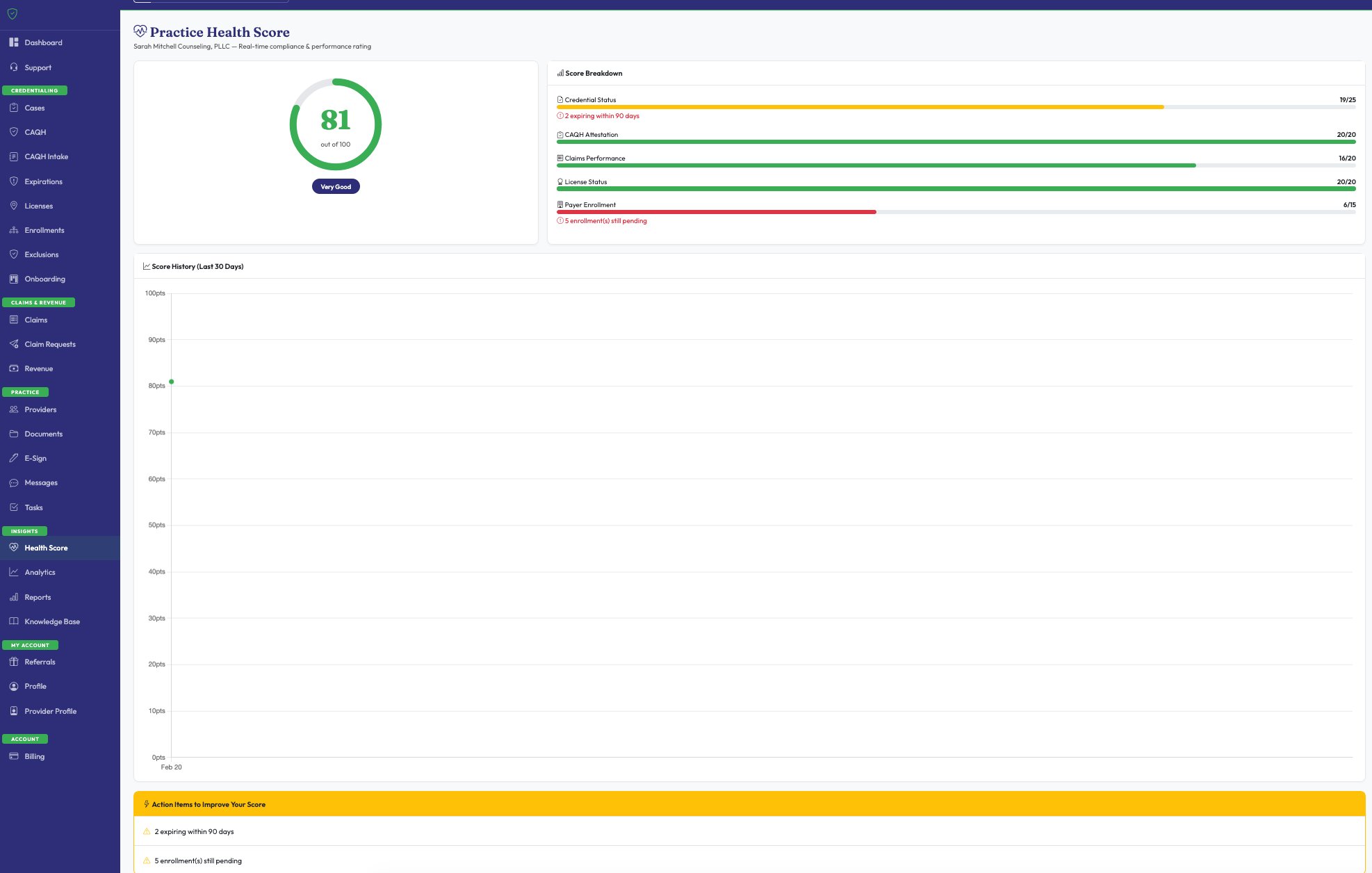
Track every dollar of insurance revenue earned through FPC — trends, payer breakdowns, collection rates, and payments. We're the only credentialing company that shows you this.

Most credentialing companies stop at enrollment. We go further — submitting claims, tracking approvals and denials, filing appeals, and showing you exactly what each payer is paying.
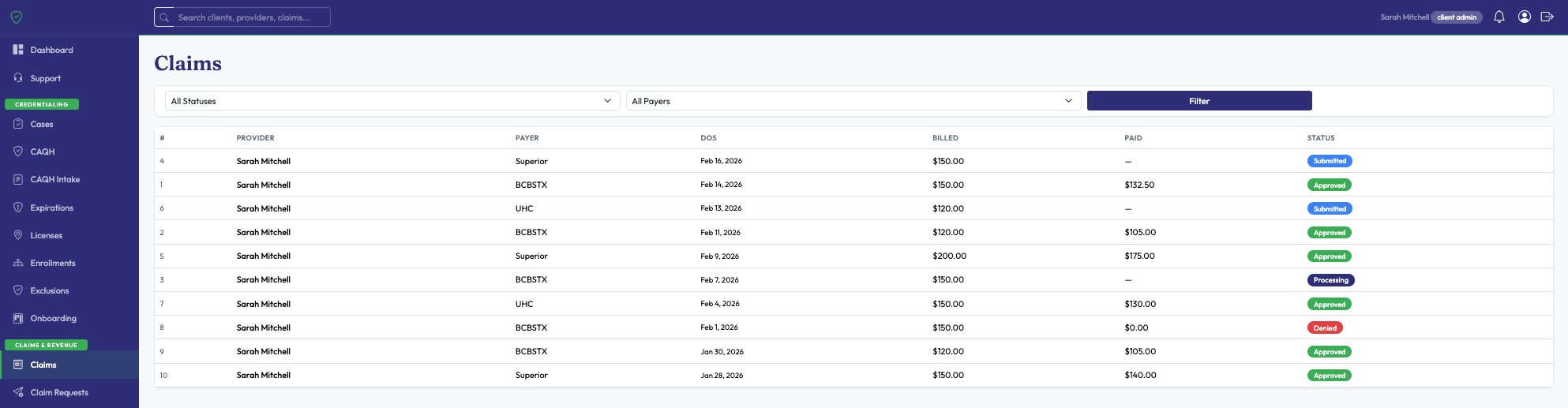
Fill in the patient details, CPT codes, and payer — our team handles the rest through Availity or Optum within 2 business days. No more navigating complicated payer portals yourself.

8 guided sections replace the 40-page paper CAQH application. Save as you go, pick up where you left off, and submit when ready.

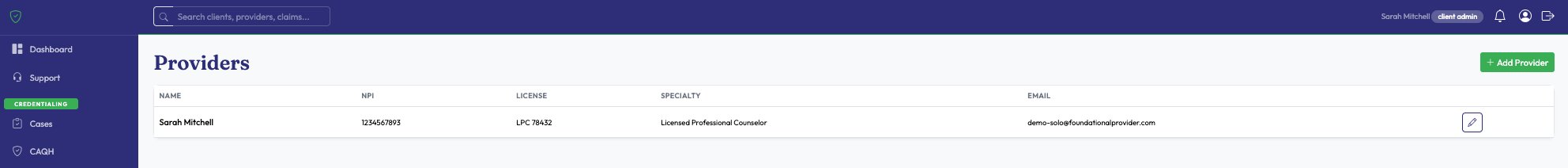
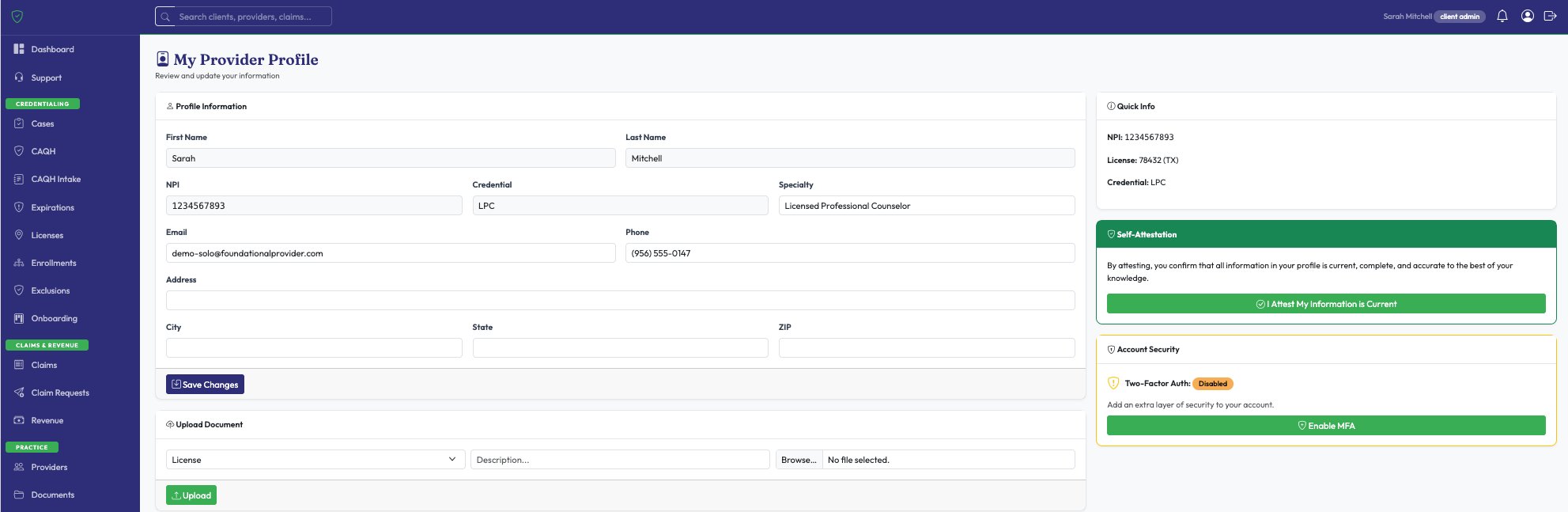
Every provider with NPI, license, specialty, and contacts in one place. Add individually or bulk import via CSV. Each provider gets a self-service profile to keep their info current.
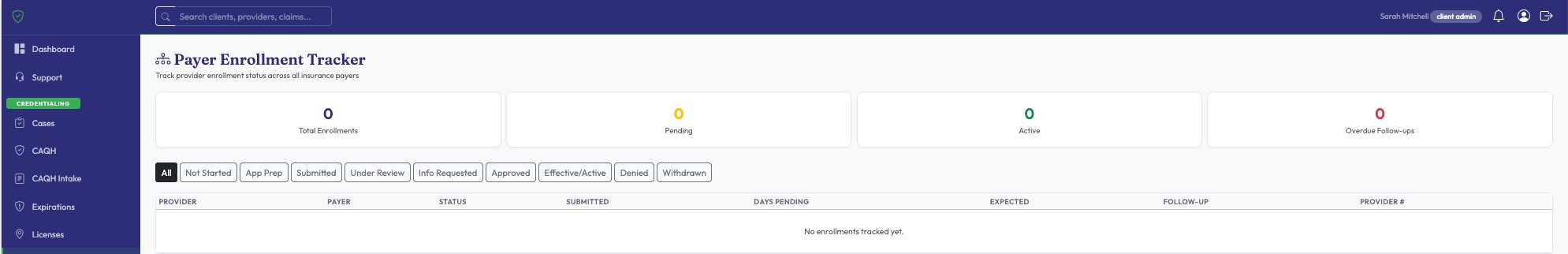
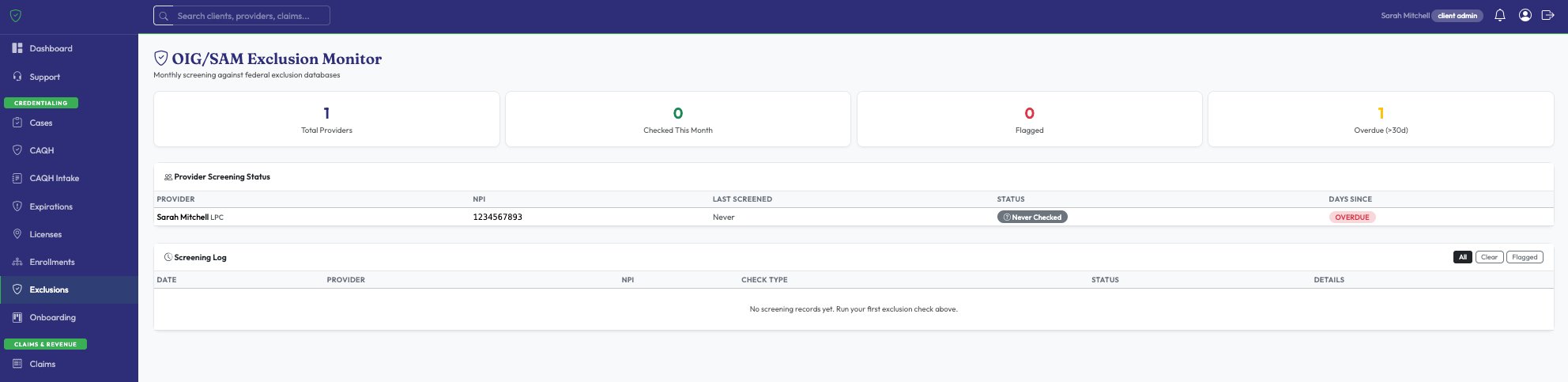
Track payer enrollments through every stage. Screen against federal exclusion databases monthly. Monitor multi-state licenses for telehealth compliance.
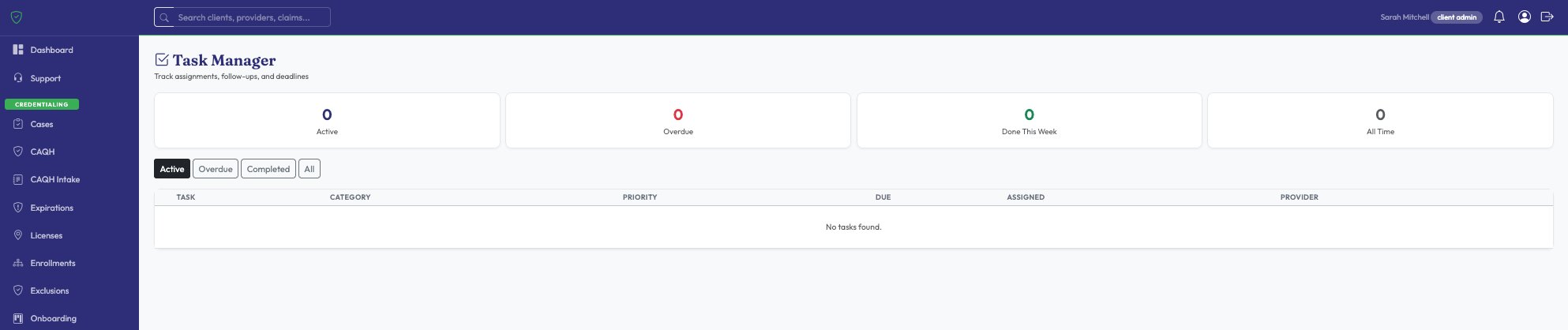
Track every new provider from intake to billing-active through a visual pipeline. Manage tasks with assignments, priorities, and due dates so nothing slips through the cracks.

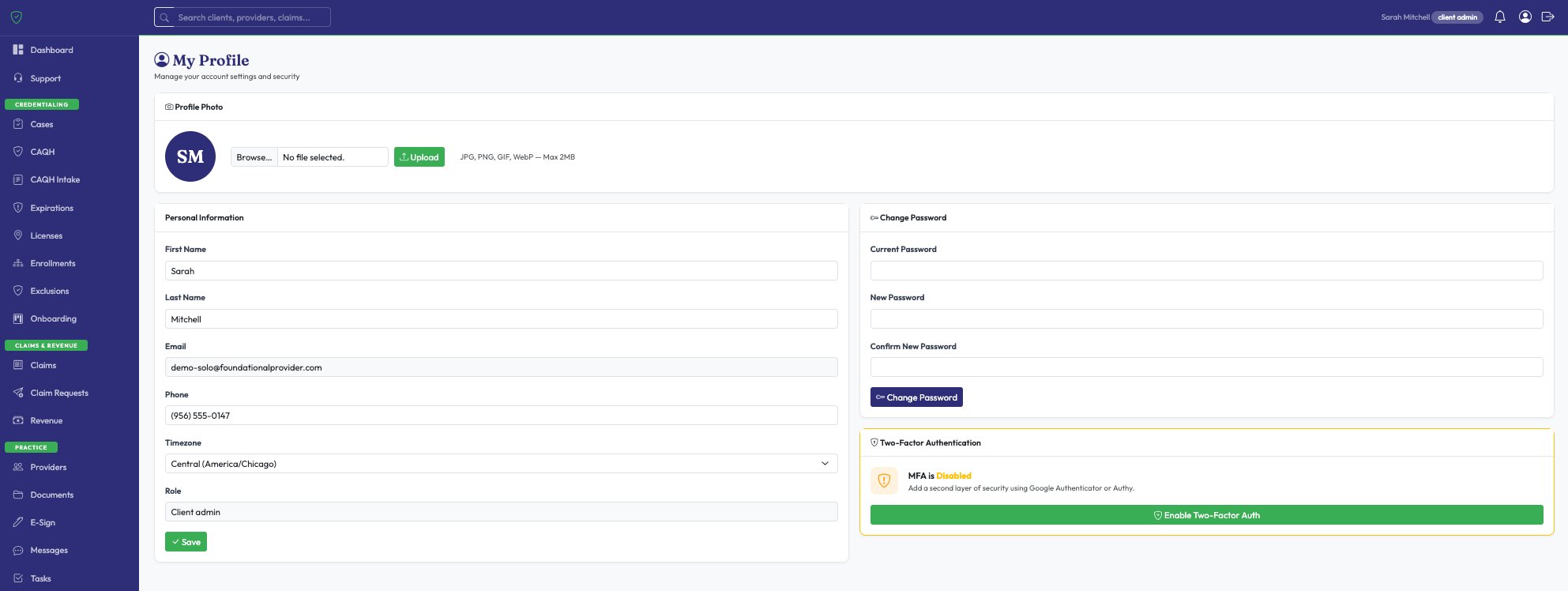
Manage your subscription, update your profile with two-factor authentication, and submit support tickets — without picking up the phone.

30+ guides on CAQH, credentialing, claims, and payer requirements. Plus — refer a provider and you both get $100 off your next month. Your unique referral link makes sharing easy.
Your most-used tools, one click away
Check your compliance score
→ 💰Track insurance revenue through FPC
→ 🔔Licenses and certs coming due
→ 📋Status on all payer applications
→ 📤We submit within 2 business days
→ 📚CAQH, credentialing & payer guides
→ 🎁You both get $100 credit
→ 💬Submit a ticket or check status
→Other credentialing companies use spreadsheets and email chains. We built something different.
Automated emails at 90, 60, 30, 14, and 7 days before any credential expires. Nobody else does this.
No more emailing to ask "where's my application?" Log in anytime and see every case, document, and deadline.
The only credentialing company that shows exactly how much insurance revenue you've earned through us.
A 3-month delay can cost a solo provider $40,000+ in lost insurance revenue. Start your free trial and get moving today.